It’s getting depressing. It’s as though nothing ever changes, and maybe nothing ever does. Regular readers probably remember the Disneyland measles outbreak four years ago. As bad as that outbreak was, however, it was an outbreak that made the impossible possible with respect to vaccinating; in its aftermath, spearheaded by Sens. Richard Pan and Ben Allen, California passed SB 277, a law that eliminated nonmedical exemptions to school vaccine mandates. SB 277 was approved by the California legislature in June 2015 and signed into law by Governor Jerry Brown on June 30, 2015. The new law took full effect in the 2016-2017 school year, and it has worked. Nonmedical exemptions have plummeted. That’s not to say that the law is perfect. Unfortunately, there’s a huge loophole in that any physician can write a letter in support for a medical exemption. Not surprisingly antivaxers have taken advantage of that weakness in the law, namely that there is no overriding governmental body that reviews and approves requests for medical exemptions, as there is in, for example, West Virginia, where requests for medical exemptions are reviewed by an Immunization Officer, who determines if they are appropriate “based upon the most recent guidance from the Advisory Committee on Immunization Practices (ACIP), the American Academy of Pediatrics (AAP), and the American Academy of Family Physicians (AAFP) with respect to medical contraindications or precautions for each vaccine”.
As a result, medical exemption rates have increased, thanks to an increase in medical exemption requests, some likely organic from parents who found it easier to claim nonmedical exemptions than going to the trouble of claiming a medical exemption, but also due to bogus medical exemptions on sale from a cottage industry of antivaccine quacks like Dr. Bob Sears, who blazed the trail.
Unfortunately, we’re in the midst of multiple new measles outbreaks, the largest occurring in Washington, across the Columbia River from Portland, Oregon. As a result, the same battles from 2015 are taking place in 2019, this time with antivaxers rallying in a state with a major measles outbreak to oppose a bill that would eliminate personal or philosophical exemptions to requirements families immunize their children against measles, mumps, and rubella (MMR), led by—who else?—Robert F. Kennedy, Jr. and the usual cast of characters. This bill isn’t even as comprehensive as SB 277 in that it wouldn’t eliminate religious exemptions, but antivaxers are still fighting it with all they have. Of course, you can predict what will happen if this bill passes; antivaxers will all get religion.
As history repeats itself—whether this time as farce or not, I’ll leave the reader to decide, although arguably everything antivaxers do is infused with farce—there are other elements that keep repeating, in particular, the claim that measles is “not that big a deal” or “just a childhood disease.” You might remember the brain dead argument that because there was an episode of The Brady Bunch that made a joke about the kids getting measles, it must mean that doctors didn’t think measles was dangerous back then. It is, as I like to call it, the Brady Bunch fallacy. But is this true? The answer, obviously, is no.
The dangers of measles, take one: SSPE
Of course, I’ve discussed the dangers of measles before here on Respectful Insolence many times. For instance, the complications of pneumonia, encephalitis, and perhaps the most feared complication of measles, subacute sclerosing panencephalitis (SSPE), a universally fatal complication in which the measles virus lies dormant in the brain, only to reactivate on average 7-10 years following the measles infection. As Steve Novella described it, SSPE leads to “severe brain inflammation. SSPE causes widespread damage to the brain. It usually starts subtly with changes in behavior, problems at school, difficulty walking, and muscle twitching. As the disease progresses it causes seizures of increasing frequency and severity, and progressive dementia. Eventually the disease leads to coma and death, on average 1-2 years from onset of symptoms. The disease is universally fatal and without any cure.” The risk of SSPE after measles had been estimated at one in 100,000, but it turns out that children who get the measles before age 5 could have as high as a one in 1,387 chance of developing SSPE, and kids who get the measles before age 1 could have a one in 609 chance.
It turns out that a “rare” complication of measles is not as rare as had previously been believed.
The dangers of measles, take two: a new study
Basically everyone, even the antivaccine movement, concedes that the measles vaccine is highly effective at preventing the measles. Actually, there are a few who don’t, but most simply try to argue that measles isn’t deadly and that therefore the fantastical “risks” ascribed to the vaccine by antivaxers (autism, neurodevelopmental disorders, diabetes, sudden infant death syndrome, etc.) outweigh the benefits of presenting measles. Be that as it may, the point is that the main benefit of vaccinating for measles has generally been believed to be the not-insignificant benefit of preventing the measles and its attendant complications, including the most dreaded SSPE. However, a new body of evidence is developing that the benefits of preventing measles go beyond just preventing measles and its known complications. In fact, it turns out that vaccinating against measles lowers all-cause mortality among children.
A new study adds to the growing evidence that measles is even more harmful than traditionally thought, making measles vaccination even more important than believed. From Science Daily:
In the largest study to date on children in a low/middle income country, new research in Ghana finds that the timing of a measles vaccine in an overall vaccination schedule can have a profound impact on child survival rates beyond protecting against measles infection. The findings, published today in open access journal Frontiers in Public Health, suggest that measles vaccination in the recommended sequence may have made an important contribution towards achieving the Millennium Development Goal 4 of reducing child mortality.
Frontiers in Public Health
Here’s the study. Basically, it followed yearly cohorts of children aged 9-23 months from 1996 to 2012. The study area was the Kassena-Nankana East and West Districts in the Upper East region of northern Ghana, which have an estimated population is 160,000 of whom about 8% of the current population is aged 9–23 months. The area is quite large, covering a land area of 1,675 km2. Its major health care facilities include a hospital that serves as a referral hospital to seven health centers, a private clinic, and over 40 Community Health Compounds located in rural communities and manned by trained nurses who provide basic health care as well as routine vaccinations. The area is mostly rural (80%) with the primary occupation being agriculture.
Before we get to the results, here’s some background on the current vaccination schedule in Ghana and its history that will help put those results into context. The current schedule in Ghana includes one dose of Bacille Calmette–Guerin (BCG) at birth, four doses of oral polio vaccine (OPV) (at birth, 6, 10, and 14 weeks), three doses of pentavalent (Penta) vaccine (at 6, 10, and 14 weeks), two doses of rotavirus at (6 and 10 weeks), three doses of pneumococcal vaccines (at 6, 10, and 14 weeks), two doses of measles (at 9 and 18 months), and one dose of yellow fever (at 9 months). Note that Penta vaccine (diphtheria, tetanus, pertussis, Haemophilus influenza type b, and hepatitis B) was introduced in January 2002 to replace diphtheria–tetanus–pertussis (DTP), and in May 2012, three additional vaccines, pneumococcal, rotavirus, and second dose measles vaccine (MV), were added to the vaccination schedule for 18-month-olds.
For this study, a total of 38,333 children were assessed for survival in relation to the measles vaccination status within the first 12 months from interview date and until 5 years of age, using Cox proportional hazards models. The findings were quite striking. In essence, measles vaccine (MV), after the third dose of diphtheria-tetanus-pertussis (DTP, or DTP3), is associated with a significant decrease in all-cause mortality in the children in this cohort.
With that background, here are the details:
Children not vaccinated with MV at enrollment had 38% higher risk of dying than those vaccinated with MV-after-DTP3 during 12 months of follow-up [HR = 1.38 (1.15–1.66)] (Table 2). When mortality was assessed from interview date until 5 years of age, measles-unvaccinated children had 22% higher risk of dying than children vaccinated with MV-after-DTP3 [HR = 1.22 (1.05–1.41)]. The size of the beneficial effect of MV did not change when we censored for measles deaths (Table S1 in Supplementary Material).
Stratifying the analysis by periods in which DTP and Penta were used, children without MV in the DTP period (1996–2001) had 30% higher risk of dying in the first 12 months of follow-up [HR = 1.30 (1.04–1.62)] than those who received MV-after-DTP3. In the Penta period (2002–2012), children without MV had 52% higher risk of dying during 12 months of follow-up than those who received MV after Penta3 [HR = 1.52 (1.12–2.05)] (Table 2). The risk associated with not receiving MV did not change when we censored for measles deaths (Table S1 in Supplementary Material). When the children were followed from the assessment date until they were 5 years old, children without MV during the DTP period had 10% higher risk of dying than those with MV after DTP3 [HR = 1.10 (0.92–1.32)]. In the Penta period, children without MV had 44% higher risk of dying than those who received MV after Penta3 [HR = 1.44 (1.13–1.84)] when they were followed from the assessment date until they were 5 years old. The risk of dying for MV-unvaccinated children was higher during the Penta period compared to the DTP period in the first 12 months after assessment of vaccination status (52 vs 30%) (P = 0.021), and with follow-up to 5 years of age (44 vs 10%) (P = 0.005).
The most important qualifier in the results discussed above is this: “The risk associated with not receiving MV did not change when we censored for measles deaths.” In other words, even though the measles vaccine protects against measles, it protects against more than just the measles. Those who didn’t die of the measles were still protected by the measles vaccine from other causes of death:
We, further, classified the MV-unvaccinated children into two groups; children who received other vaccines but not MV, and those who did not receive any vaccine (unvaccinated). The adjusted HR for those who received other vaccines except MV compared with MV-after-DTP3 vaccinated children was 1.42 (1.18–1.72) in the first 12 months after assessment of vaccination status and 1.24 (1.06–1.44) with follow-up to 5 years of age.
So basically, the measles vaccine was the key, with decreased mortality associated with its receipt after DPT3. The authors looked for potential confounding factors, such as “general improvement in the health-care delivery system, health literacy as well as infrastructure, which could have affected the mortality rates and also increased MV coverage.” They also conceded that the comparison group of no measles vaccine “may represent the population with no access or difficult access to vaccines or health care, hence have higher mortality in general.” However, they pointed out that they still observed much higher mortality among MV-unvaccinated children compared with MV-after-DTP3 in “both communities with nurses and control communities without nurses” and that the “difference between the two groups disappeared making it unlikely that the difference in mortality is primarily due to inherent weaknesses or frailty.”
Overall, the results of this study clearly demonstrate a nonspecific benefit to measles vaccination, but the mechanism is unclear, particularly given the inconsistencies noted with previous studies, which the authors freely discuss:
Our results point to a beneficial effect of MV on child survival. The 38% higher mortality for MV-unvaccinated children would correspond to 28% lower mortality for MV-vaccinated children. Considering that this estimate is probably conservative, this is consistent with other studies from developing countries which have reported mortality reductions in the range of 30–86% (3, 6). Other studies comparing mortality rates before and after the introduction of MV reported major reductions in mortality after the introduction of MV (3, 28–31). The data from the present study also supported that MV may have non-specific beneficial effects which go beyond protecting children from dying from measles infection.
Measles vaccination was associated with beneficial effect for both boys and girls before receiving any campaign vaccine (Table 4). However, after the campaigns, we found a significantly stronger beneficial effect of measles vaccination for boys, but not for girls. It is unclear why the beneficial effect is stronger for boys as many other studies reported stronger beneficial effects of measles vaccination for girls than boys. For example the SAGE review suggested that MV had a 40% (22–53%) stronger effect for girls than boys (6). However, some studies have suggested that OPV is associated with stronger beneficial effects for boys than for girls (32, 33). Hence, we recommend that future studies examine the sex-differential effect of measles vaccination on all-cause mortality before and after OPV or measles campaigns.
I noticed this sex-associated difference as well, because I remembered a study from 2015 that I discussed, which observed the same thing (a decreased mortality in children vaccinated against the measles that couldn’t be explained by just its effect on measles incidence) but with a more marked effect among girls. The hypothesis supported by the study was that measles infection causes an immunomodulation/immunosuppression that lasts around three years after the infection and that can lead to increased mortality from other infectious diseases. Other studies are less clear-cut in terms of a mechanism, but several studies show an association between vaccination against measles (and a few other diseases) with decreased all-cause mortality.
Vaccines: More powerful than believed?
If “all” that vaccination did was to decrease deaths from infectious disease, they would still be the most effective preventative medicine ever conceived by the human mind, but it turns out that they might do even more than just prevent the diseases they are designed to prevent. Michael J. Mina hypothesized a mechanism in 2017:

A lot of this is speculative in that we don’t really know for sure how the measles vaccine contributes to decreased non-measles-related mortality. We just know that, even after eliminating confounders, a beneficial effect remains. We also know that this these beneficial nonspecific effects (NSEs) might occur with other vaccines, as the authors of the current study note:
Previous studies have suggested that OPV might have beneficial NSEs (32, 35, 36). Findings from a randomized trial suggested that OPV might have beneficial non-specific effects that reduced all-cause mortality by 17% (30). Though the underlying biological mechanisms have not been fully studied, some studies suggest that OPV, just like BCG, is capable of inducing strong immune training (36). In this study, the NID campaigns with OPV or MV might have reduced the effect of being MV-after-DTP3 vaccinated vs MV-unvaccinated.
As has been shown for BCG, beneficial NSEs may be due to epigenetic changes reprogramming innate immunity. This may change once the child gets a new vaccination (19, 20). The specific immunological mechanisms behind the non-specific effects of vaccine are still being investigated, and it might be a mixture of heterologous immunity, trained innate immunity, and other types of changes in the immune system (16, 19).
The irony, of course, is that antivaxers frequently (and loudly) claim that vaccines harm the immune system when, if these hypotheses hold up, it would appear that exactly the opposite could well be the case. Vaccines actually do “stimulate the immune system” in beneficial ways, and those benefits could well go beyond just preventing the diseases intended to be prevented. They might even prevent type I diabetes, too.


142 replies on “The benefits of vaccinating against measles go beyond preventing measles (2019 edition)”
Thank you for keeping publishing on this topic.
Re: the claim that measles is “not that big a deal” or “just a childhood disease.”
Doctors, the CDC, Orac here on this blog, etc, kept telling us, way back in 2000 and before, that measles has a death rate of about 1 per 1000 and will come back if the vaccinal coverage keep falling down. They were called pharma shills and fearmongers by antivaxers, exaggerating the effect of a silly little childhood disease.
Fast forward to the 2010’s years. Measles epidemics across the North America and Europe, every few years (the cyclic part is starting to look eerily like in the 1930’s, isn’t it?)
The WHO numbers for 2018, in Europe, are about 41,000 cases of measles and 37 recorded deaths. i’m sure the readers can do the ratio.
And the direct deaths are just the tip of the iceberg. As Orac reminds us, measles is accompanied of suffering, sequels and co-morbidities. Just the immune-suppression / immune amnesia effects may result in a small cascade of other viruses doing better at infecting people.
Reality has a nasty way of saying “told you so”.
European countries also had extremely high rates of hospitalizations. This Italian summary puts theirs at over 40% (and supports your point about deaths). http://www.epicentro.iss.it/problemi/morbillo/bollettino/Measles_WeeklyReport_N33eng.pdf
link = Errore 404 (pagina non trovata)
They’ve changed the url for that pdf.
It is now at:
http://www.epicentro.iss.it/morbillo/bollettino/Measles_WeeklyReport_N33eng.pdf
/ measles is “not that big a deal” or “just a childhood disease.”
Nah, nothing to worry about. WHO just says that there “in 2017, there were 110 000 measles deaths globally, mostly among children under the age of five”.
Sounds pretty harmless to me, at least if we are comparing it to the black death or the Spanish Influenza epidemic in 1918–1919.
Gotta love how anti-vaxxers love to prattle on and on about how “naturally” catching horrible diseases like measles can strengthen the immune system (while of course completely ignoring the risks of infection–e.g. the Philippines is reporting this morning 136 deaths, mostly in children, from their measles outbreak (with many thousands of cases) due to under vaccination). Anti-vaxxers, with their rigid flat-earther minds, are unable to fathom that the immune system could be strengthened without the infection risk by vaccination.
Indeed. As I’ve said several times before, catching a disease to gain immunity to it is like burning something to fireproof it.
Accepting vaccine contraindications to gain community immunity is like adding a spark to something that burns. The goal of vaccine continuous improvement is to eliminate contraindications so no one gets hurt (e.g., additional pre-vaccine screenings).
@ Julian Frost,
I won’t need to say this several times.
“additional pre-vaccine screenings”
For what specifically?
It will be good not to read this vapidity any more.
Well, before vaccination, there was variolation. While it worked, it also quickly vanished into the history books when the better alternative came around.
Dr Chris:
I know how much you love Dr Bob Sears – so here is a tasty morsel for you:
he appeared today on Null’s show ( see PRN.fm) to educate the audience about measles, vaccination and mandates and yes, it was as bad as you can imagine ( maybe even worse)
He speaks at approximately 32, 40 and 44 minutes into the woo-fest ( there is other BS by the host and guests. My input is intended to save you from as much of the usual dreck as possible- which is my function here)
I wonder if he said anything that breaks his.. um … parole here.
Being on the show alone should be enough I’d guess: enabling a well known disease promoter
The California Medical Board is as useful as teats on a bull when it comes to Sears. They clearly have no spine or teeth.
I’m not entirely sure where the idea that “getting these diseases naturally” is considered beneficial. Any disease is a shock to the system, much like the Spanish Flu causing a healthy immune system to go into overdrive & ultimately lead to further complications (like pneumonia) which killed people in less than 24 hours.
It all just smells like disease-apologists trying to justify their decisions not to vaccinate. A few things here too – in any outbreak, it is the children of anti-vaxers who usually suffer first, followed by the vulnerable (babies too young to vaccinate and the medically-fragile). Containing these outbreaks cost millions of dollars (in many cases) – and it annoys me to no end that anti-vaxers try to claim these diseases were never feared before vaccines, when parents lined up for blocks to get their kids vaccinated when these vaccines were first released.
Ugh, I can’t believe that we’re talking about this in 2019.
“where the idea that “getting these diseases naturally” is considered beneficial”
sigh
You are thinking like an immunologist, not a layman.
It’s a remnant from pre-vaccine culture.
Since most people only get childhood diseases once, then it is beneficial to get them. Once it’s done, it’s done. Hence, pox parties.
Assuming the child survives, of course.
That was not so long ago. When I was born, the only vaccines really given routinely were smallpox and polio. And the BCG. And I’m not that old.
Add to it the long-lasting belief that natural infection is longer-lasting than vaccination. Heck, my highschool biology teachers believed it.
That may or may not have some true to it, but as you point, at the price of a nasty shock for the organism, plus real risks of other lasting effects. People were naturally reinfected – and thus naturally “re-vaccinated” – with the wild viruses during their life simply by coming in contact with children, so the lifelong immunity may not be lifelong, after all (my apologies, I think you know this better than me).
It’s just grandma’s wisdom passed uncritically onto the next generation. Once with a solid grain of truth, because there was no alternative, but now obsolete. Reinforced, of course, by the Natural fallacy.
I started school in 1956, and lining up for shots and smallpox vax was a regular part of school. My smallpox “scratch” wouldn’t heal for a long time and was a little pus blob for a long time. I had a little plastic (not sure it was actually plastic in those days) shield taped over it for ages, and when I complained, my Mom proceeded to tell me all about smallpox, complete with horrible pictures. If I said the polio shot hurt, I got the same with pictures of kids in iron lungs. I did have measles, mumps, and chicken pox, but my Mom was never glad about it and worried enormously about measles in particular. It was blindness she seemed most concerned about. We had to stay in our room with dark curtains the whole time.
This brings me to a question—when did MMR become available?
“We had to stay in our room with dark curtains the whole time.”
Your mom was crazy.
F68.10, that’s a rude and ignorant thing to say. Staying in a darkened room was a standard means of dealing with the photosensitivity caused by measles infection.
OK. I went overboard. Apologies. Still, it strikes me as overreaction.
My parents lived through the last decade before the measles vaccine became common….and they both had friends who went blind from the measles….it certainly wasn’t an overreaction.
@ Mimi:
I started school after you did – I don’t remember the smallpox “scratch” at all and have a minimal scar ( unlike some other kids I knew)
BUT I did get the measles: my mother made an appointment for me to get the new vaccine and had to cancel because I caught the measles in the intervening week. AS I’ve related before, I don’t remember much except that I had to stay in a dark room and couldn’t read, draw or write ( which I wanted to do very much); I know ( from much older cousins) that I missed 3 or 4 weeks of school and that my parents were worried about my vision. My grandmother must have been extremely worried about me because she hired a man to drive her to see me midweek – and she never did that even when my father was in a serious accident. I didn’t eat much so they were worried about that too- I lost a lot of weight.
The first MMR in the USA was introduced in 1971. Later another version with an improved rubella bit was approved in 1978.
And you had a very good mom.
“when did MMR become available?”
For us French, it was in the very early 80’s. A measles vaccine may have been available before, but not yet mainstream. That’s why I got the chance to experiment all “wild” versions of the childhood diseases. Including mumps, which I gave to my dad (I guess his natural immunity waned)..No harm done, but we could have done without.
Mimi, I am a few years younger than you, but our experiences were similar: I also got vaccinated against polio, which was probably pointless, that horse having left the barn a couple of years before.I not only got the Salk but also the Sabin vaccines. My case was only diagnosed in retrospect but some of the effects, even though relatively minor, continue to pester me even now. In addition to your list
I also had German measles, again hardly a thrill a minute.
None of those diseases was anything harmless or minor or fun to go through, unlike what the antivaxx coven continue to claim. Measles was on the whole a distinctly unpleasant experience. Having to lie in a dark room, not even permitted to read, was boring on top of everything else, but definitely not the worst of it. There’s likely no connection, but just about a year later, I had pneumonia that kept me home from school for weeks.
I count myself lucky that I never had pertussis. I think my poor little lungs would have taken it as a final insult and just quit on the job. Diphtheria was feared but pretty much unseen in that time and place.
Unlike some other places that gave BCG vaccination to children, we had tuberculosis screening by fluoroscopy at the county health center.
All in all, the status of infectious disease was very different then, and most definitely not better. I dodged several “bullets”.
Oh and just by the way, the only vaccine I had had at the time was smallpox, and I turned out to be autistic without the alleged “help” of MMR, or any of the other alleged villains.
https://vancouversun.com/news/local-news/teens-defy-parents-to-get-measles-vaccine-during-vancouver-outbreak
And good for them.
Lawrence,
As a child of the advent of polio vaccines in the 50’s I remember crowds of parents at the mass vaccinations. They would have rioted if the vaccine had run out. No fear in the past, yeah!
Robert Estrada
Orac writes,
It’s getting depressing.
MJD says,
A decade ago, Michael J. Dochniak wrote about the non-beneficial specific effects (NSEs) of vaccines that may induce regressive autism (e.g., cross-reactive antibodies based on protein homologies, neurotrophin overexpression from the degranulation of mast cells, memory B-cell specificity and expression) and thereafter is labelled an “American Loon” and “Antivaxer.”
Today, Michael J. Mina writes about how similar immunological mechanisms from vaccines may induce beneficial nonspecific effects (NSEs); making vaccines “more powerful than believed.”
Q. Does the yin and yang of NSEs continue to make vaccines a polarizing subject.
@ Orac,
It’s depressing when labels (e.g., American Loons, Antivaxers) are used to describe individuals who pontificate on the non-beneficial specific effects (NSEs) of vaccines.
The existence of beneficial NSEs doesn’t presuppose the existence of non-beneficial NSEs.
“The existence of beneficial NSEs doesn’t presuppose the existence of non-beneficial NSEs.”
The reverse is also true. Without even looking at the evidence, it is not unrational to believe that all these effects at least cancel themselves out in terms of benefits/non-benefits. Leaving out herd immunity at the predominant effect of vaccines.
Beneficial NSEs as well as non-beneficial NSEs are in the end not really meaningful in the broad picture of things compared to the benefits of herd immunity.
“Without even looking at the evidence, it is not unrational…”
It is to me. Apart from a very rare anaphylactic reaction and a just as rare vaccine-induced case of polio from OPV, what non-beneficial NSEs are there?
“It is to me.”
Good for you.
Most people do not look at the evidence. I’m just claiming that even from this perspective, you do not have to exaggerate fears, as for every cherry-picked fear, there’s likely a benefit that has been overlooked. It’s better not to look at evidence if you’re bound to cherry-pick things to fit your own biases.
“Michael J. Mina writes about how similar immunological mechanisms”
No, he doesn’t.
He doesn’t prance around in a latex costume and pretends he is a scientist.
To start with, he is a real scientist. To continue, his hypothesis is build on the existing body of scientific knowledge. There is no need for “and then a miracle happen” to explain it.
Notice that MJD today perseverates on a name that ONLY PARTIALLY resembles his own as he did recently with Dr DG and a guy with the same surname. Both examples illustrate an unique way of focusing on discrete parts rather than on the totality or on meaning: showing how his mind works.
“A decade ago, Michael J. Dochniak wrote about the non-beneficial specific effects (NSEs) of vaccines that may induce regressive autism” says MJD. That only goes to show that you have been pumping out swill longer than I would have guessed/
The dochniak continues to distimm the doshes.
@ Denice Walter and Old Rockin’ Dave,
It’s an echo from my inventing and patent writing days wherein creating and defining terms was a means to overcome prior art, and an examiner’s objection/rejection. The patent process can really affect the thinking process (e.g., Albert Einstein-Clerk at the Swiss Patent Office in Bern).
Ok, ok, let’s set aside that we’re still dealing again with Africa, and where there are many other susceptible factors that may hamper a child’s health and making him extra vulnerable to diseases. Let’s set aside this fact, and consider that measles vaccination is doing these amazing things. Then what?! What exactly is the cost benefit analysis, outside of the spin that the vaccine is extremely safe? Will three rounds of MMR that prevent 1 in 1000 deaths (again we’re assuming this is the rate for the developed world) offset 2 in 100 developing permanent brain damage, or 1 in 10 with ADHD, or 1 in 40 with LD? Oh wait — in fairness, those harms are coming from the entire schedule. Do tell then what is the true cost of three rounds of MMR vaccination as they relate to those mentioned injuries. What factor should we divide by? Or is it all a package deal thing, where once you choose MMR you must accept all the other vaccines –kinda like how there is no separate measles vaccination option?
In what imaginary universe does this happen, Greggles?
What are you talking about, moron? The 1/1000 death rate is happening in European countries as well, not just in Africa.
Last time I checked, we didn’t suddenly burst a sewer or something, so it’s not a degradation of hygiene.
Go ahead, make my day. Try to say that Americans have a more balanced diet than Italian or French people.
Well, you’re not completely useless, Greggles. That’s a beautiful example of “begging the question”.
“Then what?”. F*ck off Greg. Jerks like you are bringing these diseases back.
Don’t blame me, Christopher. And don’t blame Wakefield, Del, Facebook, Russian bots, and so on and so on either. The blame instead can be placed squarely on one basic equation…
A rash that goes away in a few weeks < permanent brain damage
Christopher, the other stuff are just variables that essentially have no bearing on that equation. I’ll let you get back to your job, Christopher. A job that literally upholds that equation.
No Greg, I do blame you and all the other anti-vax scum like you that are dumber than dirt and lie like rugs and don’t give a crapy when people die from these diseases while you continue to spew your unfounded lies about vaccines. You’re too cowardly to put your name out here, and we all see the reason for that. You’re all cowards.
Greg: “A rash that goes away in a few weeks < permanent brain damage”
I just watched the movie “The Rider.” It is a must see, especially for anyone who does not understand the difference between brain damage and autism. What makes it very interesting is that the characters with brain damage and autism play themselves.
It actually based on true events, though modified to about 60% true, and 40% not so much: https://en.wikipedia.org/wiki/The_Rider_(film)
The point that this study will be downplayed as sample set being from non-first world region shouldn’t be disregarded entirely. It is a limitation of the study.
Once again, Gerg assumes facts not in evidence.
@ MarkN
That’s true, indeed. Malnutrition and similar factors decreasing the immune system efficiency are well known for making people more susceptible to diseases and more likely to recover poorly. That would extend to other ill effects of a measles infection, and may be a factor in the observed extra benefits of vaccination.
I haven’t the full article at hand, I wonder if the authors addressed these concerns?
We could also look ourselves at the health/food level of the countries where the study took place. Africa is really big. There is Somalia, and then there is Senegal. More differences than between, say, Russia and Spain.
My hastily point, above, is that the difference between the measles outcomes in North American/European countries and third world countries is not to the point of “everybody survive unscathed”/”everybody die” (like, say, for leprosy – access to antibiotics does make quite a terrific difference in that case).
It’s more of a “a little less likely to suffer/die” / “more likely to suffer/die” situation.
Myself, earlier:
“I haven’t the full article at hand, I wonder if the authors addressed these concerns?”
Duh. Apologies for my laziness. I went back reading Orac’s post and he already quoted parts of the article relevant to my question.
The short answer is apparently, yes.
Nothing of thia is true. Vaccines does not cause autism (and autism is not brain damage). Start with telling us why twin studies are wrong.
Arno
I don’t think you will ever get Greg to stop using the them “brain damage”. Anti vaccine pundits claim that children with autism were neuro typical till they were vaccinated. If they use any other term to describe people on the ATS they are tacitly admitting that vaccines don’t cause autism. So they are stuck with the term.
This raises the question are the brains of people with autism in any way structurally different to thoes who aren’t on the spectrum?
No, and one especially pathetic part is that he’s just trying to claw his way onto the bandwagon. Here.
“This raises the question are the brains of people with autism in any way structurally different to thoes who aren’t on the spectrum?”
Neural connectivity tends to be different, though it’s not a universal rule that you will find biomarkers.
The differences are more meaningful when viewed from a cognitive science perspective (i.e. theory of mind for instance) than from an anatomic/neurophysiological perspective.
Congratulations. Your racist card is officially issued.
This is the guy who said in the recent Boyer thread that autism is worse than anything done by any totalitarian regime/imperialistic country/dominant group around the globe during the 20th century (and even maybe before), both in harm done individually and general scope.
I think the card was already off the press.
How is racist to point out that Africa is largely an underdeveloped continent, and the poorer health situation of their kids makes them particularly vulnerable to diseases?
Says the wholly underdeveloped person.
Shelly, rather than give you a simplistic and misleading answer, here are a couple of links to start you on your way:
https://www.spectrumnews.org/news/autism-brains-show-widespread-alterations-structure/
https://www.quora.com/What-are-the-neurological-differences-in-an-autistic-brain-compared-to-a-neurotypical-brain
Just remember, when you have met one autistic person, you have met one autistic person, not all of us.
Grogger, do you really think that one death in a thousand cases is trivial? You’re not a parent, are you?
Let’s look at this statistic another way. If you received a credible warning that there was one chance in a thousand that a sniper would pick you off as soon as you walked out of your house, you would probably pull the curtains, turn out the lights, and hide under your kitchen table, occasionally crawling across the floor for the most urgent necessities, and that would not be overreacting..
Or try this: How about the odds of being struck by lightning? They’re pretty small, unless you walk out on the golf course in a thunderstorm under a steel ribbed umbrella. The actual odds don’t increase by all that much, but it’s probably not the kind of risk you’d want to take, and you would be right not to take it.
Not vaccinating your child to face one chance in a thousand of death, not to mention somewhat greater risks of other morbidity, Not vaccinating your child is a gamble with the life of your child as the ultimate possible loss, and worse, it’s not your life to gamble with.
ORD, that scenario doesn’t lend to a straight answer since I would have to consider two other factors. First, are there any mitigating circumstances that may influence that 1 in 1000 risk? For instance, what if that shooter has a dislike for unhealthy, immune compromised people and tend to shoot them more? If that’s not me, I might not worry so much. Also ORD, if I hear news that the shooter is not on my.block, I might also not worry.
Second ORD, I would consider the side-effects of hiding. Will hiding under the kitchen table give me a 2% chance of brain damage, 10% of ADHD for hiding in the bathroom, 20% chance of LD for hiding under the bed, and so on and so on. ORD, considering these side-effects of hiding, can you see why I might even opt to take that 1 in 1000 chance with the shooter?
There was a recent CBC piece on the measles outbreak in Vancouver BC and part of the interview with the public health official cited that measles vaccination rate in Canada was in the order of 80%. I was shocked and appalled! Another article mentioned that low rates occurred in wealthy areas like W. Van because of hesitancy and in E.Van because of poverty. The one upside is that there is increasing coverage of the dangers of the anti-vax crowd and their misinformation. It is good to see mainstream media calling out anti-vaxxers, finally!
Well at our clinic in Vancouver public health has been swamped with requests and calls from worried parents scrambling to get the MMR today
That is great to hear! People forget how much fun vaccine-preventable diseases were to us who were kids back in the day. I particularly fondly remember getting my tonsils out and then getting mumps right after that. Good luck to your vaccine clinic and I hope the momentum keeps up!
And another good thing, is they have barred 33 students and staff from going anywhere near the schools until they have proof of vaccinations being up to date, and that due to the outbreak and the corresponding vaccination scramble, the confirmed rate is now 95%.
Still some are refusing, but thankfully they won;t be able to send their pox ridden spawn into the general school population.
And this is quite interesting. Considering we’re well below that magical herd-iimmunity threshold (particular emphasis show be placed on ‘magical’), why is the sky not falling here in Canada? Surely the bodies should be piling up everywhere and even around our neighbourhood Tim Horton’s.
That average number obscures a lot of local variation, let’s pick on Quebec – vaccination rates vary from mid-60 to 93%. So there are pockets of potential for epidemics. Back in 2011, Quebec had over 700 measles cases in one of the largest outbreaks in N America. Measles is considered eradicated in Canada since the late 90s so cases nowadays represent imported measles but since 2002 the number of cases and incidence rate has been increasing. It is still low but this seems to be more dumb luck than anything else. There is too much complacency out there as the diseases have waned and the urgency to avoid them has waned as well. The Quebec outbreak got as large as it did partly because doctors didn’t recognize early cases and delayed quarantine helped the spread. Prevention of disease is always preferable to suffering through it, in my opinion. Being old enough to have suffered through them, I would have preferred to avoid those experiences.
“why is the sky not falling here in Canada”?
Because infection by viruses is a stochastic process. Nothing magical in that, much less in the thresholds that are post-hoc constructs.
Not really. Simple SEIR models are governed by two PDEs. One can add corridor effects, etc.
It seems like there’s four ODEs in the SEIR model. Not two PDEs.
http://www.public.asu.edu/~hnesse/classes/seir.html
Stochastic versions of such models have been developed.
https://arxiv.org/pdf/0910.4443.pdf
Anyhow. Does anyone know how the herd-immunity thresholds are estimated. Do they use such models? Or not?
It used to be $\latex 1-1/R_0$, with $\latex R_0$ being the basic reproduction number, but things are a bit more complex.
One more try (I haven’t had coffee yet):
It used to be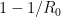 , with
, with 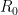 being the basic reproduction number
being the basic reproduction number
@Narad: thank you.
I think the ODE version assumes perfect mixing; I’m not sure what I was recalling with the two PDEs, but I have to beat it out of the library soon.
^ Ah. You can get it down to two for SIR models because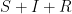 is constant.
is constant.
Actually, heading into my local Tim Horton’s today, I saw two men lying on the ground in front of the store. My heart sunk thinking that maybe I spoke too soon. I rushed to one, asking him if he came down with something and was reeling from Canada’s poor vax rate. He looked up at me confused, but also asked if I could spare change. Oh well — at least I thought of helping.
Antivaxers commonly shrug off the toll of vaccine-preventable diseases in developing countries. You see, it’s their fault for being dirty and malnourished.
There’s never any sense of responsibility for their own propaganda helping to limit vaccine uptake in the Third World.
Orac: “Basically everyone, even the antivaccine movement, concedes that the measles vaccine is highly effective at preventing the measles.”
Except the more than a few antivax loons who claim that measles vaccination spreads measles (promiscuous shedding by the vaccinated, doncha know).
Which is interesting considering that this concession does not sit well with our cause. What concession that does not sit well with their cause is the vaccine pushers prepared to make?
There has been a real, dramatic increase in cases of autism?
By order of logic, a finding that vaccines can trigger a fever and that fever can cause autism is one way in which vaccines can cause autism?
Outside of thimerosal and MMR the autism-vaccination connection could be studied further, and even if an unvax/vax study is unethical a well designed retrospective study could assist?
William Thompson confession does not sit well with reassuring parents about the safety of vaccines, and we should have him testify in front of Congress to set the record straight?
Any takers? Again, who are the ones devoted to a religion and the protection of it?
You actually said a specific thing, fever causes autism, though you did not cite anything. If this were true, measles would cause even more autism, because fever is more serious. Rubella does cause autism, but this is by interfering brain development.
“a well designed retrospective study could assist”
Already done. Your side never liked them and forgot them immediately.
“who are the ones devoted to a religion and the protection of it?”
Is it a trick question?
With your antivaxer pals, it is always, always, the vaccine.
Doesn’t matter if the vaccine is live-attenuated, dead pathogens, bits of pathogens build in yeast, if it has thimerosal or aluminum salts, is single-illness or multivalent, given to toddlers, teenagers or adults. Heck, even vit-K injection at birth is sometimes amalgamated within the vaccine schedule.
It is always, always, the vaccine.
Link?
@Greg: its foolish to assume that the rise of the rates of autism is due to vaccination when a much simpler explanation (Ockham’s razor) exists: (1) better detection and diagnostic procedures and (2) increased perimeter of the diagnostic criteria (not restricted any more to Kammer style autism).
Science has advanced and rightly identified autism a spectrum wider than initially assumed. Along with cognitive therapy that has done much more for the autism population than meds and institutionalization.
Let’s recognize progress for what it is.
“link?”
Alain kindly provided plenty of them one month ago. Specifically to you.
And you repaid him with your usual passive-agressive snide comments.
Well said. All too often the antivaccine fundamentalists and evangelists suck up all the oxygen in the room whenever any autism-related topic is discussed.
I say fundamentalists meaning that they pulled their “science” out of their fundaments.
F68.10, also well said. Sadly, it’s too logical for Grogger and the other members of his coven to process.
Gotta love the current antivax meme making the rounds, about how Hep B vaccination supposedly damages the brain (based on a Chinese study in neonatal mice).
Problem is, the same researcher they’re wildly praising also co-authored a study showing (again in mice) that flu vaccination early in pregnancy enhances brain development of the wee rodents. So J.B. Handley undoubtedly will now urge pregnant women to get their flu shots.
Or not. 🙂
A campaign against hep B vaccination will definitely claim lives in a very visible manner. Back in the day we used a very rough rule of thumb, the Three Ones.
One percent of the infected would die straightaway. Another one percent would go on to develop liver cancer and nearly certainly die of it. Yet another one percent would suffer such longterm damage, such as cirrhosis, that they would die of it.
The real stats are different, but it was a good way to keep us thinking about the consequences in our patients, as well as the risks to ourselves of carelessness.
It’s been 8 years since “Melanie’s Marvelous Measles” was published. Perhaps it’s time for a sequel? I’m thinking “Melanie’s Melancholic Mortality” or “Melanie’s Murderous Mom”? Or how about “Melanie Is Dying From SSPE Because Her Idiot Parents Wouldn’t Vaccinate Her, And All The Carrot Juice And Melon In The World Didn’t Help”.
I’d forgotten about that book Factotum.
There’s a fairly new antidote, published last year, ‘Pablo tiene sarampión’, a free downloadable PDF book, which now has an English translation, ‘Paul has measles.’ Expertly written, with good illustrations featuring a clearly uphappy schoolboy and a two-fanged paramyxovirus. The original Spanish book was written by three Mexican virologists from the Mexican Virology Network.
Livre (PDF) disponible aussi en Français! (‘Paul a la rougeole’).
English translation was edited by doyen of US virology Vincent Racaniello, from TWiV. Final product beautifully done. I’d love to see hardcopy versions of this book, as it would be ideal for medical clinics. Sorry I don’t have a download link.
This Paul has measles looks like the English version.
The copyright seems to be with the authors and RED MEXICANA DE VIROLOGÍA . Since they have released it as a free PDF, they probably would not mind if various clinics printed and bound their own copies. Probably an email or two would get permission.
With a good colour printer and access to someone’s binding machinery it would be pretty easy. Staples Canada seems to sell an adequate binding machine for under $CDN 150.
How about “Susie’s Sensational Syphilis”? “Dan’s Delightful Dengue”? “Luanne’s Lovely Lhassa Fever”? “Ethan’s Excellent Ebola”? “Harold’s Happy Hepatitis”?
It’s just a gift that keeps on giving.
If I remember, Sarah Visits a Naturopath was the follow up.
We could also say neuro impaired?
@Greg: Autism is both often impairment/disability and also “neurodiversity” (I hate that term more than its semantics). One does not preclude the other.
<
blockquote>
No Greg, I do blame you and all the other anti-vax scum like you that are dumber than dirt and lie like rugs and don’t give a crapy when people die from these diseases while you continue to spew your unfounded lies about vaccines. You’re too cowardly to put your name out here, and we all see the reason for that. You’re all cowards.
And what a specimen you are Mr Hickie! So well educated, so professional, so ‘principled’, so ‘ethical’ —- and also so wrong. I seriously don’t know whether to pity you or laugh. Sit down big fella, you’re starting to make a fool of yourself!
Tough and timely editorial in the Charlotte Observer, calling for an end to phony religious exemptions to vaccination.
“Objections to vaccinations also are not based on science, which has regularly and thoroughly debunked the notion that vaccines are unsafe. Despite that, anti-vaxxers stubbornly shake their head, fueled by an internet-based patchwork of falsehoods and suppositions. Their recklessness not only endangers children who have legitimate medical exemptions, but adults who have vulnerable immune systems because of chemotherapy and other treatments.”…
“It’s time to treat vaccination deniers for what they are – a threat to others.”
@Dangerous Bacon: “It’s time to treat vaccination deniers for what they are – a threat to others.”
Does that mean they should be involuntarily committed to a psychiatric hospital? Sounds like it.
That is quite the strawman.
“That is quite the strawman.”
I know. Couldn’t resist the rhetorical question. I plead guilty.
While I think the AV cultists are a danger to others, some of the rhetoric coming from the side of fact, reason and evidence, are becoming a bit unhinged themselves at times, a lot of people are starting to call the AV cult a terrorist organisation I note, and that just makes us on the side of reason, facts and evidence not look too dissimilar to the loons in AV cult at times and I caution against it.
Speaking of terrorism, I particularly liked the fake vaccination campaigns in Pakistan.
https://www.bmj.com/content/343/bmj.d4580
At least real terrorists have sounder arguments than antivaxers, if you can fathom their perspective.
I don’t know that they are the “side of fact, reason and evidence”, rather lay people who are just starting to realise that anti-vaxx is a thing. I am disturbed by the comments I see celebrating “Darwin Awards” and wishing a pox upon the anti-vaxxers houses. That is saying something given my own occasional aggressive disposition. But yes, unhinged pro-vaxxers don’t do public health initiatives any favours.
Yes, Mr Bacon, the antivaxxers are the ‘worst menace’ to public health and enough is enough; it’s time to kick ass, but whose ass are you going to kick? That mom who drank your kool-aid and now wants blood? How about that dad who loves vaccines and also hates the ‘antivaxxers’, but after considering some of his kids’ ‘issues’ and talking things over with the pediatrician it has been decided to go ‘slow’?
With the vaccination war, I am often amused at the simplistic imagery that’s being conveyed. One would gather that there are two teams battling on the pitch in different coloured uniforms, and their names clearly emblazoned on the back of their jerseys.
“How about that dad who loves vaccines and also hates the ‘antivaxxers’, but after considering some of his kids’ ‘issues’ and talking things over with the pediatrician it has been decided to go ‘slow’?”
He just has to deal with the facts that his kid may putatively get hurt, but that it’s for the greater good. Period.
Stuff happens. That’s how things work.
How very trollish of you.
Both trollish and factual. Again, I plead guilty.
Thing is no credible pediatrician worth their salt would ever be giving nonsensical information that would turn someone who already accepts the evidence that vaccines are safe (they just are, get over it) so why would such a conversation ever happen, the only place I see the kind of rank misinformation aimed at clouding the good judgement of parents in in mums groups and rabid AV cultist groups
F68.10 might benefit by reading this passage in the editorial again.
“(Antivaxers’) recklessness not only endangers children who have legitimate medical exemptions, but adults who have vulnerable immune systems because of chemotherapy and other treatments…
“It’s time to treat vaccination deniers for what they are – a threat to others.”
@Dangerous Bacon: What did I misunderstand?
That antivax ideology is indeed a threat to others and should be addressed (as the editorial proposes) by eliminating phony religious exemptions.
If you can show me anything in the editorial suggesting involuntary psychiatric commitment for antivaxers, I’ll buy you a kewpie doll. Or even a free session with your analyst. 🙂
Well, being a “threat to others”. Can I have my kewpie doll?
Hmmnn! Is F68.10 ‘Management’s’ new PGP? The over-the-top provaxeer that says crazy stuff and needs to be corrected by the regulars. Oh — and this proves how ‘reasonable’ the regulars are!
@Greg: no.
We work this all the time with woo-bies.
One of us says something outrageous, then others rush in to “correct” him/her, thus “proving” we’re much more decent and reasonable than the off-the-wall sorts that frequent antivax forums.
It fools ’em all the time. Greg is the first one to catch on to the game. 🙁
My own bias is the following: I know from personal experience within my family that one can get overcarried into medical madness by following blindly some doctors. While what we’ve been experiencing was a curious mixture of woo blended with real medicine gone astray, I have developed rather negative instincts towards medical claims in general. Had I not been resolutely pro-science thanks to my upbringing, I’d have fallen full-face on alt-med as did some members of my family. So basically, I’m pro-science, I feel severely burnt down by real medicine and am more distrustful of it than I should be, but I really have full-fledged hatred of woo meisters. And specifically of woo meisters that have made their cuckoo’s nest within the medical profession, earth’s worst scum.
At least I’m aware of what my biases are and what my proclivities are.
I’m simply outraged that the scientific criticism of vaccines, which may sometimes be legitimate, has been hijacked by the autism “debate”. It’s not only disgraceful and harmful to both herd immunity and antivaxxer’s kids, but also cloaks the serious issue of autism in more dark clouds than it ever should be. I’m pissed off.
That’s said.
“ I have developed rather negative instincts towards medical claims”
Wait, what?
Your ‘nym is a derivative of the International Classification of Diseases (ICD) 10 F68.10 (a reimbursement billing code for claiming treatment of a personality disorder [factitious disorder imposed on self, unspecified]).
Synonyms of irony: odd, strange, weird, peculiar, incongruous; sound familiar to you?
@Moose: reality can be more complex than what you can read hastily in a ICD-10 classification code. I won’t solve the riddle for you: I’d be writing a 10 page essay, or worse, a book, to explain all that.
@Moose: I hadn’t noticed that the code has been revised in 2019. I was using the sense of it before the 2019 revision, the one that was valid in 2018. Maybe that should give you a clue.
Nope, if I go any further into publicly revealing your self-diagnosed psychopathology you’ll accuse me of violating HIPAA.
Still, by admitting that you instinctively revile medical claims despite your medical claim-related ‘nym you melted down IronyMeter. I bought it from Orac’s on-line store for $999.99 Canadian + shipping (or 79¢ US). Sure, I could have bought it cheaper on Amazon (or EBay) but I wanted authenticity (and Orac threw in a free “Vaccines Cause Adults” coffee mug).
I accept both PayPal and Apple Pay.
@Moose: “you melted down IronyMeter”.
Thank you. Very much flattered.
I’m a bit broke for the moment with all these medical bills, so I’m afraid I’ll have trouble replacing your IronyMeter ®.
https://www.skepticalraptor.com/skepticalraptorblog.php/anti-vaccine-terrorists-time-call-them/
Holy cow, polarizing the vaccine safety debate to the extreme.
@ Orac,
Is the phrase “anti-vaccine terrorist” legitimate? Please advise.
I doubt that Orac will respond. So I will.
What is a terrorist anyway? A bomber? A shooter? Or someone who spreads ideas that may trigger others’ violent actions? Someone whose beliefs indirectly lead to the death of innocent people?
I suppose that it could be argued either way but personally, I like liars and killers better
BECAUSE anti-vaxxers lie about the “inefficacy and dangers” of vaccines in order to scare people
and, when they frighten vulnerable young parents into not vaccinating, either the unvaccinated child or another medically fragile person could die.
Unfortunately, no one can directly link anti-vax leaders to specific deaths.
(It should be noted that television stations are discussing TODAY how violent rhetoric from the right influenced a white power advocate into stockpiling weapons and planning assassinations of liberal politicians and news people
.I wonder if he read Mike Adams/ Alex Jones?)
C’mon provaxxers, have a heart and don’t accuse me of being a terrorist! Imagine if you have your way, and I were to land in the slammer with ISIS’s Omar. How the hell would I compete with that rap sheet?!
Omar explains, ‘I am here because I beheaded infidels. I threw them from tall buildings and blew them up as they walked along their streets. I held their women as slaves and abused them. You Greg, why are you here, brother?
Greg explains, ‘I posted antivaccine stuff on the ‘net.’
Omar shrinks in respect, ‘Brother, I did hear about your kind, but never thought I would have the honour of meeting you in person.’
@Greg: move to Pakistan. You can have the best of both worlds: islamic militants gunning down polio workers.
https://www.bbc.com/news/world-asia-31507217
Hi, well; how weird. On Saturday I wrote a post on a vaccine topic thread (large message board forum that I’m a regular poster on) to say: “You know what I’d like to see from Gorski? An analysis of Peter Aaby’s research.”
So, thank you? I’m a huge fan of Aaby’s work. He’s not afraid to call it how he sees it.
For those here yammering about “dangerous antivaccine ideology”: Seriously. If you are that terrified of the Measles (yes. I know a dangerous disease) then vaccinate. I have one child dead within 12 hours of vaccination & one child permanently & severely disabled following a dosage mistake of a vaccination. I have paid my dues & I owe your herd nothing. Needless to say; none of the herd has ever come knocking at my door to offer any help.
You will never change those you call antivaccine because most of them are either; 1. Like me. Or; 2. Don’t want to be me. Unless … you were to stop agreeing with everything you are told & use some critical thinking. Admit there is room for improvement. Like Aaby. You’re too afraid to do that because it’s an admission of some sort.
Post references or it didn’t happen. So sick of random anti-vaxxers showing up claiming nonsense without any citations acting so damn high and mighty
I believe Christine is referring to this 2018 article:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5868131/
WHO commented on this topic in 2014:
https://www.who.int/immunization/sage/meetings/2014/april/3_NSE_Epidemiology_review_Report_to_SAGE_14_Mar_FINAL.pdf
It seems both parties squabble over the directions of biases.
Effects seem weak, biases are unclear, not replicated.
Thanks to F68.10 for sharing those references.
I had dug through the first one before and noticed a couple things. The uncertainty bounds of practically all the comparisons encompass 1.0, so while it shows an increased risk, that risk is not statistically significant. Also the number of children and percentages who died in each group are very similar. The difference which leads to the increase in risk is in the number of person-years followed after the initial examination. For some reason, the vaccinated children who died did so sooner than the unvaccinated children. Since we don’t know cause of death, it is hard to speculate on why this happened.
And because this is a small study with only a few hundred children as compared to the 38,000 in the Ghana study, it is prone to larger statistical variations. And since these results were not replicated in the several studies in the WHO analysis, it is probably just a statistical fluke.
That doesn’t stop the antivax squad from trotting it out repeatedly because it gives them a result which matches their claims, the very definition of confirmation bias.
If you are done patting yourself on the back for your “enlightenment” and actually use that to apply some critical-thinking skills yourself, you’d know that this statement is a load of bollocks. All of us support continued vaccine safety monitoring and improvements to vaccine platforms and safety profiles. Perhaps you know that but feel better about yourself attributing false notions to us. Or maybe not. Aaby’s work is important but requires a way to go and it is just plain stupid for anti-vaxxers to use it as a weapon. You are the ones who cause investigators pause about this kind of work because they know how you people abuse it.
Do you live in Guinea-Bissau? Do you trust thirty year old data from one of the poorest countries on this planet? (hint: many children die from effects of bad sanitation there).
I guess you know Aaby is one of the authors of the study being discussed. Which was in Ghana, a country with a much better economic climate than Guinea-Bissau.
Boy, anti-vaxers like to use 3rd World statistics when it suits their purposes, but then utterly reject them because “Not America.”
Did you go to Vaccine Court ? What was the verdict ?
@Greg I want to hear what Walter Thompson would say under the oath. Lying to antivaxxer is not a crime, perjury is.
If you are really interested in vaccine safety, do some Google Scholar queries:
hpv vaccine phase ii 38400 hits
hpv vaccine phase iii 33200 hits
hpv vaccine post licensure 7200 hits
saline placebo vaccine 35400 hits
Aarno, I find you an interesting case. Debating provaxxers, I very rarely get the impression that they believe their own BS. Don’t get me wrong, I do believe that the gullible masses who have swallowed the propaganda hook, line and sinker do believe vaccines are safe and effective. As to those peddling the propaganda and are knowledgeable on the issues, you guys, I don’t for a second sense this. I would wager big dollars that you would all fail a lie detector test.
Then there is something about you, Aaarno. A certain perseverance and desperation to confront me. I start considering, is Aarno for real, does he he really believe the lie? Maybe some autistic people have too much on the line to ever consider they were duped. Are you autistic Aarno?
PS: Christopher Hickie sometimes comes across as convincing, but the giveaway with him is the irritability. Though he excuses it as his frustration with the menacing antivaxxers, the feeling that is left is you’re still dealing with a professional. A professional whose skills extends farther than pediatrics and in the area of mendacity.
“Maybe some autistic people have too much on the line to ever consider they were duped.”
Seriously?
I see that Gerg has found his hamster wheel.
In case anyone needed more evidence that, any opinions of vaccines aside, Greg is a terrible person: “Maybe some autistic people have too much on the line to ever consider they were duped. Are you autistic Aarno?”
1) That’s super abelist.
2) He’s using autistic as a slur and a terrible thing to be. Which feeds back to point 1 above.
6D10.2
You send a comment and I answer it. Have you some problem with that ? I am trying to get an argument out of you,but you just rant. I am not desperate at all
I figure the reason antivaxers keep regurgitating lies when they’ve repeatedly been given good evidence that they’re false, is because they feel justified in engaging in tit for tat.
They’ve convinced themselves so thoroughly that health care workers, government agencies, researchers etc. are lying to them that they feel entitled to lie in return, to combat the Giant Conspiracy.
Pro-immunization advocates on the other hand are handicapped by their unwillingness to engage in deception campaignsa along with refusal to deal in absolutes, while antivaxers feel no such compunction.
Ok, ok, I see you are a little sour about this so I’m giving you guys license to engage in deception campaignsa. Orac, are you listening?! From here on, I am giving you permission to write hateful, inane blogs. Feel free to use whatever over-the-top ad-homs, strawmen, red-herrings and outright dishonesties at your discretion. Wait!! Ok – never mind.
Indeed. Those things are the prerogative of antivaxxers.
Feel free give an actual argument to us. For starters, let us argue about genetic basis of autism.
MMWR says hi.
[…] yes. The old claim that measles is not a serious disease. It is, and it’s more serious than commonly thought. As I like to say, The past and present rebuke […]